March 28, 2025
All three main Mayo Clinic campuses have installed the most advanced clinical 7T MRI scanners. The new systems use innovative technology that greatly enhances signal homogeneity and enables patient-specific pulse transmission.
"These upgrades allow us to address some of the biggest challenges of clinical 7T imaging," says Erik H. Middlebrooks, M.D., a neuroradiologist at Mayo Clinic in Jacksonville, Florida. "We have seen enhanced image quality across several MRI sequences and reduced imaging times."
7T imaging is highly challenging technically. Mayo Clinic neuroradiologists have pioneered its clinical use to improve care for patients with epilepsy, multiple sclerosis (MS), neurodegenerative disorders, cerebrovascular disease, amyotrophic lateral sclerosis (ALS) and other neurological conditions. As a tertiary center, Mayo Clinic has a team of experts — including physicists and experienced technologists — able to provide cutting-edge patient imaging.
"Leveraging all this expertise is instrumental to the success of our 7T MRI program," Dr. Middlebrooks says.
'Remarkable' performance
Several challenges have constrained the adoption of routine clinical 7T MRI — most notably, the heterogeneity of radiofrequency transmission. "That's not much of an issue with 3T MRI. But it's very detrimental at ultrahigh field strengths, where heterogeneity can cause large variation in image signal and contrast," Dr. Middlebrooks says.
To overcome that challenge, the new 7T MRI scanners employ dynamic parallel transmission. That technique uses multiple independent transmit coils to precisely control the radiofrequency field across the imaged region, allowing for real-time adjustments to the pulses based on specific patient characteristics. That, in turn, mitigates signal inhomogeneities and improves image quality. The new 7T MRI scanners are the first use of parallel transmission approved by the Food and Drug Administration.
"Using parallel transmission safely requires predicting local specific absorption rates while simultaneously optimizing the homogeneity of radiofrequency transmission," Dr. Middlebrooks says. "That has meant lengthy calibration scans, which aren't feasible in a clinical setting."
Dr. Middlebrooks and colleagues recently evaluated a new method to solve this issue. Their approach uses precalculated, universally optimized parallel transmission pulse designs, followed by an optimization process tailored to patient-specific maps of magnetic fields. "The process is time efficient, so using this technology in routine clinical work is practical," Dr. Middlebrooks says. "The performance we've had with parallel transmission is pretty remarkable in patients with a variety of head shapes."
 Upgraded 7T
Upgraded 7T
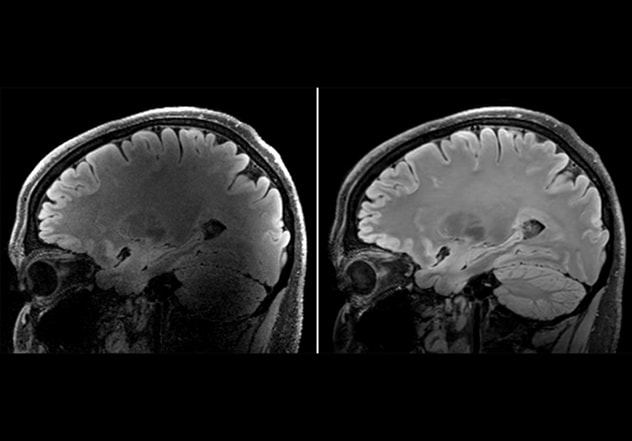
High-resolution, 0.7 mm 7T sagittal 3D FLAIR SPACE acquired in traditional single-transmit mode with conventional reconstruction (left) shows poor signal uniformity and signal-to-noise ratio. Repeat scan implementing dynamic parallel transmission and deep-learning based reconstruction (right) illustrates the reduction in signal loss, as well as improved signal-to-noise ratio.
Another significant breakthrough is using deep learning for image reconstruction. Deep-learning reconstruction methods have been used previously with 3T MRI. But increased heterogeneity at ultrahigh field strength complicates adjustment scans, adversely affecting image quality. Acquiring sufficient datasets to train deep-learning models also has been an issue. That's because training data without image acceleration can be impractical at the high resolutions possible with 7T. To train the model, the system's developers applied new deep-learning methods to fine-tune reconstruction algorithms on a smaller dataset of accelerated images from 1,000 patient datasets.
At Mayo Clinic's campus in Florida, deep-learning and dynamic parallel transmit technologies have been implemented in many commonly used clinical sequences, including magnetization-prepared rapid gradient echo (MPRAGE) and sampling perfection with application-optimized contrasts using different flip angle evolution (SPACE).
"This new technology is particularly helpful for detecting small lesions in patients with epilepsy or MS and small brain tumors," Dr. Middlebrooks says. "It enables monitoring of microscopic-level changes in ALS. Shorter scanning times also facilitate imaging of patients with movement disorders who are challenged to hold still in the scanner. The new technology unleashes the capability envisioned for 7T MRI."
MR physics expertise
Mayo Clinic's MR physicists play a key role in realizing the potential of 7T MRI. "Expertise in MR physics ensures that the scanner operates at optimal performance," says Xiangzhi Zhou, Ph.D., a medical physicist at Mayo Clinic's campus in Florida. "We collaborate with radiologists and technologists to refine imaging protocols, optimize signal noise reduction and contrast, and troubleshoot technical challenges unique to ultrahigh-field MRI."
The efforts also involve developing dedicated imaging protocols for 7T MRI. "Tailored protocols help mitigate issues introduced at higher field strengths, ensuring consistent and clinically useful imaging results," Dr. Zhou says. "Custom protocols are also necessary to accommodate novel techniques, optimize acquisition times, enhance patient exam efficiency and address specific diagnostic needs across neurological conditions."
Dr. Middlebrooks cites the upgraded 7T MRI — particularly its use of deep learning — as one of the biggest breakthroughs he's seen in his career. "It allows us to go incredibly fast, with very little penalty to image quality," he says. "But there is a definite level of skill and training necessary to perform this work. We hope that the experiences of Mayo Clinic will allow this technology to be seamlessly integrated into practices around the world in the near future."
For more information
Refer a patient to Mayo Clinic.