March 28, 2025
Mayo Clinic is expanding its use of photon-counting-detector (PCD) CT to optimize the management of neurological conditions. The cutting-edge technology provides vastly improved resolution in patient imaging.
"We can image down to in-plane resolution of 110 microns, or the width of a human hair. It's a revolution in CT imaging," says John V. Murray, Jr., M.D., a neuroradiologist at Mayo Clinic in Jacksonville, Florida.
Available at all three Mayo Clinic campuses, PCD CT is used to optimize:
- CT angiography (CTA) for neurovascular care.
- Otological imaging.
- Imaging of head and neck cancers, including pituitary adenomas.
- Identification of cerebrospinal fluid (CSF)-venous fistulas.
- Postsurgical spinal imaging.
- Deep brain stimulation (DBS) for movement disorders.
- Stereoelectroencephalography (stereo EEG) for epilepsy.
Mayo Clinic physicists play a critical role in applying this technology to patient care. "We collaborate with our team of physicists to optimize our imaging protocols," Dr. Murray says. "Our physicists are not only innovating and advancing the science. They're helping us daily with patient care."
Profound impacts for patients
 Detailed visualization
Detailed visualization
3D volume rendered imaging of a stent demonstrates the enhanced detail obtained from photon-counting-detector CT (left) compared with conventional CT (right).
Conventional CT entails a two-step conversion process. X-ray photons are first converted into visible light and then converted, as an aggregate, into an electrical signal. In contrast, photon-counting detectors directly count each photon to characterize its energy.
"The big leap with photon-counting-detector CT is that each photon is individually converted to an electrical signal proportional to its energy. That leads to huge advantages," Dr. Murray says. "We can obtain ultrahigh spatial resolution without a dose penalty. There are fewer artifacts, temporal resolution is very fast, and we can obtain high-quality scans with lower doses than traditional CT. We can also do spectral imaging, which helps differentiate between materials with similar densities."
 Avoiding unnecessary treatment
Avoiding unnecessary treatment
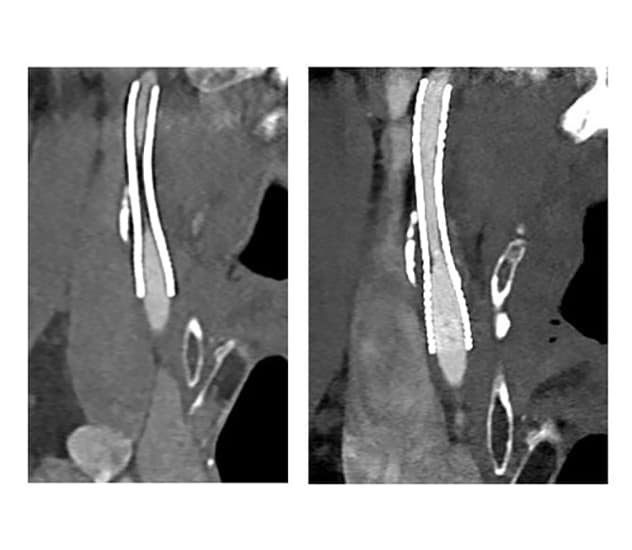
Conventional CT of a stent within a patient's cervical internal carotid artery (left) indicates possible high-grade stenosis, which would require angiogram and endovascular treatment. Photon-counting-detector CT performed the following day (right) shows the stent is clearly open.
The impact on patient care is profound. PCD CTA can differentiate between cerebral aneurysm and infundibulum and provide clear imaging of stents. Dr. Murray cites a recent case when traditional CTA indicated that a patient's stent was either occluded or had high-grade stenosis. "But when we repeated imaging on photon-counting CTA, we could see that the stent was clearly open with no stenosis. That meant the patient avoided unnecessary catheter angiogram," Dr. Murray says.
PCD CT provides similarly detailed imaging of tiny head and neck tumors. Spectral imaging can be leveraged to more clearly image these tumors. Pituitary microadenomas, which can be occult on MRI, can be seen on PCD CT. The technology also is useful for imaging otologic anatomy, pathology and implants. "We can see these small structures much more clearly," Dr. Murray says. "It's been a real game changer."
That clarity also facilitates the detection of CSF-venous fistulas. Although treatable, these abnormal connections are notoriously difficult to localize. PCD CT is able to find CSF-venous fistulas that can go undetected, even on digital subtraction myelography (DSM). CT also is a less invasive procedure compared with DSM.
For postsurgical spinal imaging, Mayo Clinic has developed an imaging protocol that significantly decreases artifacts caused by metal implants. "That allows us to see clearly if there's a hardware fracture or loosening and if surgery has resulted in successful osseous fusion," Dr. Murray says.
PCD CT's artifact reduction helps better localize metallic leads in patients undergoing stereo EEG. "Each contact of the 10 to 16 electrodes we implant is clearly displayed," says Sanjeet S. Grewal, M.D., a neurosurgeon at Mayo Clinic's campus in Florida. "That enhanced clarity is valuable in delineating seizure onset zones, as it enables us to accurately correlate electrode placement with brain activity. The ability to visualize the exact positioning of each electrode helps guide surgical planning, improving outcomes and minimizing risks during resective surgery."
At Mayo Clinic physicists work closely with radiologists to optimize the use of PCD CT for these varied neurological conditions.
"The sophistication of this new technology requires testing beyond what is needed for conventional scanners," says James M. Kofler, Jr., Ph.D., a medical physicist at Mayo Clinic's campus in Florida. "The radiologists know what they would like to visualize and at what level of image quality. Physicists can assist with the technical parameters. Exploiting all the advantages of the system requires a team that includes radiologists, physicists and technologists."
That team approach is key to Mayo Clinic's model of care. "We are always looking for ways to meet the needs of our patients," Dr. Murray says. "That started with the Mayo brothers, who were committed to finding the best technology in the world and bringing it here. To this day, that's true."
For more information
Refer a patient to Mayo Clinic.