Overview
Glioblastoma
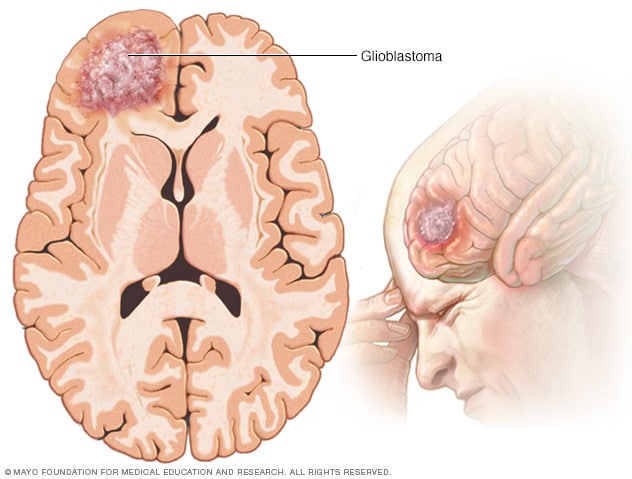
Glioblastoma
Glioblastoma is a type of cancer that starts in cells called astrocytes that support nerve cells. It can form in the brain or spinal cord.
Glioblastoma is an aggressive type of brain cancer that starts in cells called astrocytes, which support nerve cells. Because it begins in these glial cells, glioblastoma is part of a wider group of tumors called gliomas. Glioblastoma is the most common malignant form of glioma. It's the most common malignant brain tumor in adults and makes up about half of all malignant brain tumors in adults.
Within this group, glioblastoma is classified as a grade 4 glioma, the most serious type of glioma. Grade 4 means the tumor grows and spreads quickly into nearby brain tissue, which makes it hard to remove completely. As a result, these tumors can invade and destroy healthy tissue.
Glioblastoma is sometimes called GBM. The older term "glioblastoma multiforme" refers to the same disease.
Glioblastoma can occur at any age, but it happens most often in older adults. Symptoms vary based on where the tumor forms in the brain and may involve seizures or changes in thinking, speech, vision, strength, sensation or balance.
There is no cure for glioblastoma. Treatments such as surgery, radiation and chemotherapy may slow tumor growth, ease symptoms and help people live longer.
Products & Services
Symptoms
Signs and symptoms of glioblastoma can vary based on where the tumor forms in the brain.
Common glioblastoma symptoms include:
Headache and related symptoms:
- Frequent or worsening headaches.
- Headaches that are worse in the morning.
- Headaches that get worse when lying down.
- Nausea or vomiting.
Changes in thinking and memory:
- Confusion or trouble understanding information.
- Difficulty making decisions.
- Memory loss or difficulty concentrating.
Personality and behavior changes:
- Irritability.
- Reduced ability to control emotions.
- Noticeable shifts in behavior or mood.
- Restlessness and agitation.
Sensory symptoms:
- Vision issues such as blurred or double vision or loss of side vision.
- Hearing changes or ringing in the ears.
- Changes in sensation such as numbness or reduced sense of touch.
- Changes in smell or taste.
Speech and language difficulties:
- Difficulty finding words.
- Difficulty understanding language.
- Slurred or unclear speech.
Movement and coordination problems:
- Difficulty with balance or coordination.
- Weakness in the face, arms or legs.
- Weakness that affects one side of the body.
- Difficulty swallowing.
Seizures and changes in alertness:
- New seizures in someone without a prior seizure history.
- Increased tiredness or sleepiness.
- Brief periods of being less alert or harder to wake.
When to see a doctor
Make an appointment with a doctor or other healthcare professional if you have any signs or symptoms that worry you.
Causes
The cause of most glioblastomas is not known.
Glioblastoma happens when cells in the brain develop changes in their DNA. Healthcare professionals sometimes call these changes mutations or variations. DNA gives cells instructions for how to grow, divide and die.
When DNA changes occur, the instructions change. The cells may grow too fast, make too many copies or keep living when healthy cells would die. These changed cells become cancer cells.
The cancer cells can build up and form a tumor. As the tumor grows, it can press on nearby nerves and parts of the brain. It also can invade and destroy healthy brain tissue, leading to symptoms and complications.
Most glioblastomas do not run in families, and inherited causes are rare.
Risk factors
Researchers do not know why most glioblastomas develop, but a few factors have been linked to a higher risk. Factors that can increase the risk of glioblastoma include:
- Getting older. Glioblastoma is most common in older adults. But it can happen at any age.
- Being exposed to radiation. People who have been exposed to a type of radiation called ionizing radiation have an increased risk of glioblastoma. One example of ionizing radiation is radiation therapy used to treat cancer.
- Inherited syndromes that increase cancer risk. In some families, DNA changes passed from parents to children may increase the risk of glioblastoma. Inherited syndromes may include Lynch syndrome and Li-Fraumeni syndrome. Genetic testing can find these syndromes.
- Being assigned male at birth. Glioblastoma is about 1.5 times more common in people assigned male at birth.
Researchers haven't found anything you can do to prevent glioblastoma.
Complications
Glioblastoma can cause complications as it grows and affects nearby brain tissue. Which complications happen depends on the tumor's size and location. Possible complications include:
- Seizures. Glioblastoma may cause new seizures or make existing seizures worse.
- Brain swelling. Tumor growth can lead to swelling in the brain, which may cause headache, nausea or changes in alertness.
- Changes in thinking or personality. Glioblastoma can affect memory, planning, attention or behavior.
- Weakness or changes in movement. Tumors in certain areas can cause weakness on one side of the body or make coordination difficult.
- Trouble with vision or speech. Glioblastoma may affect how someone sees or speaks depending on where it forms.
- Hydrocephalus. In some cases, the tumor blocks the flow of fluid around the brain, causing a buildup of pressure.
- Glioblastoma that comes back. Even with treatment, glioblastoma often returns. When this happens, symptoms may become more noticeable and additional treatment may be needed.
Prevention
There is no known way to prevent glioblastoma. Most glioblastomas happen without a clear cause, and researchers have not found any lifestyle changes that lower the risk.
Avoiding unnecessary exposure to ionizing radiation may reduce risk, but this type of radiation is not common in daily life.