Diagnosis
Pituitary tumors often aren't noticed or aren't detected. In many cases, that's because the symptoms caused by pituitary tumors that make hormones, called functioning adenomas, and large tumors, called macroadenomas, are similar to those of other medical conditions. It's also because they grow very slowly over time. Small pituitary tumors that don't make hormones, called nonfunctioning microadenomas, often don't cause symptoms. If they are detected, it's typically because of an imaging exam, such as an MRI or a CT scan, that's done for another reason.
To detect and diagnose a pituitary tumor, your health care provider will likely talk with you about your personal and family medical history and do a physical exam. Testing to detect a pituitary tumor also may include:
-
Blood tests. Blood tests can show whether your body has too much or too little of certain hormones. For some hormones, blood test results that show too much of the hormone may be all that's needed for your health care provider to diagnose a pituitary adenoma.
For other hormones, such as cortisol, a blood test result that shows too much of the hormone may need to be followed by other tests. Those tests can show if the earlier result was caused by a pituitary adenoma or by another health concern.
Results that show hormone levels are too low need to be followed with other tests, usually imaging exams, to see if a pituitary adenoma may be the cause of those test results.
- Urine tests. A urine test may be used to help diagnose a pituitary adenoma that's making too much of the hormone ACTH. Too much ACTH leads to too much cortisol in the body and causes Cushing disease.
- MRI scan. A magnetic resonance imaging scan, also called an MRI scan, is a test that uses a magnetic field and computer-generated radio waves to create detailed images of the body's organs and tissues. An MRI of the brain can help detect a pituitary tumor and show its location and size.
- CT scan. A computed tomography scan, also called a CT scan, is a type of imaging test that combines a series of X-rays to create cross-sectional images. MRI scans are used more often than CT scans to detect and diagnose pituitary tumors. But a CT scan may be helpful in planning surgery if your health care provider tells you that a pituitary tumor must be removed.
- Vision testing. A pituitary tumor can affect eyesight, especially side vision, also called peripheral vision. Testing your eyes to check how well you can see may help your health care provider decide if other tests may be needed to detect a pituitary tumor.
Your health care provider may refer you to a specialist in hormone disorders, called an endocrinologist, for more testing.
More Information
Treatment
Many pituitary adenomas don't need treatment. They are not cancer, so if they don't cause symptoms, simply watching them over time may be a good approach. If treatment is needed, the specific treatment depends on the tumor type, size, location and growth over time. If a tumor is causing too much or too little of certain hormones in the body, that also affects the treatment. Your age and overall health play a role in treatment planning too.
The goal of treatment is to:
- Return hormone levels to a healthy range.
- Avoid more damage to the pituitary gland and restore its regular function.
- Reverse symptoms caused by tumor pressure or prevent them from getting worse.
If a pituitary adenoma needs treatment, it may include surgery to remove the tumor. Medication or radiation therapy also might be used to treat a pituitary adenoma. Treatment involves a team of medical experts. The team may include a:
- Brain surgeon, also called a neurosurgeon.
- Nose and sinus surgeon, also called an ENT surgeon.
- Hormone disorder specialist, also called an endocrinologist.
- Radiation therapy specialist, also called a radiation oncologist.
Surgery
Surgery to treat a pituitary tumor involves removing the tumor. This is sometimes called a tumor resection. A surgeon may suggest surgery if a pituitary adenoma:
- Presses on the optic nerves and limits eyesight.
- Causes other symptoms, such as headache or facial pain.
- Lowers hormone levels in the body due to pressure on the pituitary gland.
- Causes the body to make too much of some hormones.
Results after surgery typically depend on the adenoma type, its size and location, and whether the tumor has grown into tissues around it.
Surgeries to remove a pituitary tumor include endoscopic transnasal transsphenoidal surgery and craniotomy.
Endoscopic transnasal transsphenoidal surgery
Endoscopic transnasal transsphenoidal surgery
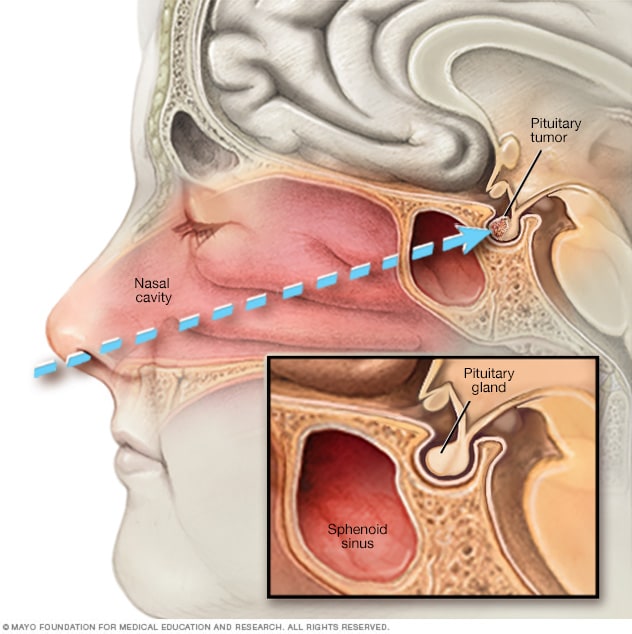
Endoscopic transnasal transsphenoidal surgery
In transnasal transsphenoidal endoscopic surgery, a surgical instrument is placed through the nostril and alongside the nasal septum to access a pituitary tumor.
This surgery also is called adenomectomy. It's the most common surgery used to remove a pituitary adenoma.
During the surgery, a surgeon — typically a neurosurgeon partnering with a nose and sinus surgeon — removes the adenoma through the nose and sinuses. The surgery doesn't require an external cut, also called an incision. It does not affect other parts of the brain. The surgery doesn't cause a scar that you can see.
Large macroadenomas may be hard to remove with this surgery. That's particularly true if a macroadenoma has spread to nearby nerves, blood vessels or other parts of the brain.
Transcranial surgery
This surgery also is called a craniotomy. It's used less often than endoscopic transnasal transsphenoidal surgery for pituitary tumors. This surgery makes it easier to reach and remove large macroadenomas or pituitary tumors that have spread to nearby nerves or brain tissue. It also makes it easier for the surgeon to see the extent of the tumor, as well as the parts of the brain around it. During transcranial surgery, the surgeon removes the tumor through the upper part of the skull through a cut in the scalp.
Endoscopic transnasal transsphenoidal surgery and transcranial surgery are generally safe procedures. Complications are uncommon. But as with any surgery, there are risks. Complications after pituitary tumor surgery can include:
- Bleeding.
- Infection.
- Reaction to the medicine that puts you in a sleep-like state during surgery This sleep-like state is called anesthesia.
- Temporary headache and nasal congestion.
- Brain injury.
- Double vision or loss of vision.
- Damage to the pituitary gland.
Diabetes insipidus
Surgery to remove a pituitary tumor might damage the pituitary gland. That can limit its ability to make hormones, leading to other medical problems including diabetes insipidus. This condition happens when the pituitary gland cannot make enough of the hormone vasopressin. That hormone is made in the back of the gland, an area called the posterior pituitary. Diabetes insipidus causes the body's fluids to go out of balance, which then causes the body to make large amounts of urine. That can cause extreme thirst and raise the risk of dehydration. Diabetes insipidus after surgery to remove a pituitary tumor usually is short term. It typically goes away without treatment within a few days. If diabetes insipidus lasts longer than that, treatment with a manufactured form of vasopressin may be used. The condition often goes away after several weeks or months.
If your health care provider suggests surgery to treat a pituitary tumor, ask about which surgery is right for you. Talk about the possible complications, risks and side effects. Ask what you can expect during recovery.
Radiation therapy
Radiation therapy uses high-energy sources of radiation to treat pituitary tumors. Radiation therapy can be used after surgery. Or it can be used alone if surgery isn't an option.
Radiation therapy can be helpful if a pituitary tumor:
- Isn't completely removed with surgery.
- Comes back after surgery.
- Causes symptoms that medications don't relieve.
The goal of radiation therapy for pituitary adenomas is to control adenoma growth or to stop the adenoma from making hormones.
Methods of radiation therapy that can be used to treat pituitary tumors include:
- Stereotactic radiosurgery. Often delivered as a single high dose, this type of radiation therapy precisely focuses radiation beams on the tumor. Although the word "surgery" is in its name, no cut into the skin is needed. It delivers radiation beams the size and shape of the tumor into the tumor with the aid of brain-imaging techniques. This requires attaching a head frame to the skull. The frame is removed right after treatment. Little radiation comes in contact with healthy tissue near the tumor. That lowers the risk of damage to the healthy tissue.
- External beam radiation. This method also is called fractionated radiation therapy. It delivers radiation in small amounts over time. A series of treatments usually is done five times a week for 4 to 6 weeks.
- Intensity modulated radiation therapy. This type of radiation therapy, also called IMRT, uses a computer that allows the beams to be shaped to surround the tumor from many angles. The strength of the beams can be limited. That lowers the risk of side effects on healthy tissue.
- Proton beam therapy. Another radiation option, proton beam therapy uses positively charged ions, called protons, to target tumors. Proton beams stop after releasing their energy within the tumor. This means the beams can be controlled to target a pituitary adenoma with less risk of side effects in healthy tissue. This type of radiation therapy requires special equipment. It isn't widely available.
Potential side effects and complications of radiation therapy for pituitary adenomas can include:
- Damage to the pituitary gland that limits its ability to make hormones.
- Damage to healthy tissue near the pituitary gland.
- Vision changes due to damage to the optic nerves.
- Damage to other nerves close to the pituitary gland.
- Slightly increased risk of developing a brain tumor.
A radiation oncologist evaluates your condition and talks with you about the benefits and risks of radiation therapy for your situation. It usually takes months to years to see the maximum benefit of radiation therapy for pituitary adenomas. Side effects and complications from radiation therapy usually don't show up right away either. It is important to have regular long-term follow-up care to detect any hormone problems that may happen due to radiation therapy.
Medications
Treatment with medications can be useful for the management of pituitary adenomas. They can help lower the amount of hormones the body makes due to a tumor. Some medications also can shrink certain types of pituitary tumors.
Pituitary tumors that make prolactin
The following medications are used to lower the amount of prolactin a pituitary adenoma makes. They also can often shrink the tumor.
- Cabergoline.
- Bromocriptine (Parlodel, Cycloset).
Possible side effects include:
- Dizziness.
- Mood disorders, including depression.
- Headache.
- Weakness.
Some people develop compulsive behaviors, such as problems with gambling, while taking these medications. Those behaviors also are called impulse control disorders.
Pituitary tumors that make adrenocorticotropic hormone
Tumors that make adrenocorticotropic hormone, also called ACTH, cause the body to make too much cortisol. That condition is known as Cushing disease. Medications that can lower the amount of cortisol the body makes include:
- Ketoconazole.
- Metyrapone (Metopirone).
- Osilodrostat (Isturisa).
Possible side effects of these medications include a heart problem that can lead to a serious heartbeat irregularity.
Another medication called mifepristone (Korlym, Mifeprex) can be used for people with Cushing disease who have type 2 diabetes or glucose intolerance. Mifepristone doesn't lower the amount of cortisol the body makes. Instead, it blocks the effects of cortisol on the body's tissues.
Side effects of mifepristone include:
- Tiredness.
- Weakness.
- Nausea.
- Heavy vaginal bleeding.
The medication pasireotide (Signifor) works by lowering the amount of ACTH a pituitary adenoma makes. It's taken as a shot twice a day. Providers typically suggest pasireotide when surgery to remove an adenoma doesn't work. It also may be used when an adenoma can't be removed with surgery.
Side effects of pasireotide include:
- Diarrhea.
- Nausea.
- High blood sugar.
- Headache.
- Stomach pain.
- Tiredness.
Pituitary tumors that make growth hormone
Two kinds of medication can treat pituitary tumors that make growth hormone. Providers often prescribe these medications when surgery to remove a pituitary adenoma hasn't worked to return the amount of growth hormone in the body to a healthy level.
-
Somatostatin analogs. This type of medication lowers the amount of growth hormone that the body makes. It also may partially shrink a pituitary adenoma. Somatostatin analogs include:
- Octreotide (Sandostatin).
- Lanreotide (Somatuline Depot).
These medications are given as a shot, usually every four weeks. A form of octreotide that can be taken in a pill, called Mycapssa, also is available. It works like the forms that are given as a shot and has similar side effects.
Side effects of somatostatin analogs include:
- Nausea and vomiting.
- Diarrhea.
- Stomach pain.
- Dizziness.
- Headache.
- Pain at the site of the shot.
- Gallstones.
- Worsening diabetes.
Many of these side effects improve over time.
- Pegvisomant (Somavert). This medication blocks the effect of too much growth hormone on the body. It's taken as a shot every day. This medication may cause the side effect of liver damage in some people.
Pituitary hormone replacement
The pituitary gland controls growth, thyroid function, adrenal function, reproductive function and the balance of water in the body. One or all of those can be harmed by a pituitary adenoma or by its treatment with surgery or radiation. This is because of the hormone changes they can cause. If your hormones fall to unhealthy levels, you may need to take hormone replacement therapy. This can restore hormones to a healthy level.
Watchful waiting
In watchful waiting — also known as observation, expectant therapy or deferred therapy — you might need regular follow-up tests to see if a tumor grows or if hormone levels change. Watchful waiting may be a choice for you if an adenoma isn't causing any symptoms or triggering other health problems. Talk to your health care provider about the benefits and risks of watchful waiting versus treatment in your situation.
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Coping and support
It's natural for you to have questions throughout the diagnosis and treatment of a pituitary tumor. The process can be overwhelming and sometimes scary. That's why it's important to learn as much as you can about your condition. The more you know and understand about your care, the better.
You might find it helpful to share your feelings with other people who are in a situation like yours. Check to see if support groups for people with pituitary tumors are available in your area. Hospitals often sponsor these groups. Your health care provider may be able to help you find the emotional support you need.
Preparing for your appointment
You're likely to start by seeing your primary care provider. If your provider thinks you might have a pituitary tumor, the next step may be appointments with specialists. Those specialists may include a nose and sinus surgeon, a brain surgeon — also called a neurosurgeon — or an endocrinologist — a doctor who specializes in hormone disorders.
Here's some information to help you prepare for your appointment.
What you can do
When you make the appointment, ask if there's anything you need to do in advance, such as not eating before having a specific test. Make a list of:
- Your symptoms, including any that may seem unrelated to the reason for your appointment.
- Key personal information, including major stresses or recent life changes and family medical history.
- Medicines, vitamins or supplements you take, including doses.
- Questions to ask your health care provider.
Take a family member or friend along, if possible, to help you remember the information you receive.
For a pituitary tumor, questions to ask your health care provider include:
- What is likely causing my symptoms or condition?
- What are other possible causes?
- What specialists should I see?
- What tests do I need?
- What is the best course of action?
- What are alternatives to the approach you're suggesting?
- I have other health conditions. How can I manage them together?
- Are there restrictions I need to follow?
- Are there brochures or other printed materials I can have? What websites do you recommend?
Don't hesitate to ask other questions.
What to expect from your doctor
Your health care provider is likely to ask you a number of questions, including:
- When did your symptoms begin?
- Have they been continuous or occasional?
- How severe are your symptoms?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
- Have you had imaging tests done of your head for any reason in the past?