Diagnosis
Diagnosing endometrial cancer
Pelvic exam
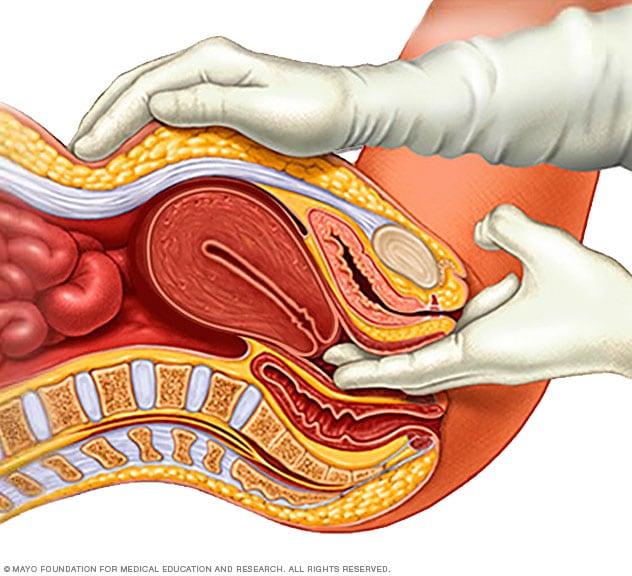
Pelvic exam
During a pelvic exam, a doctor inserts one or two gloved fingers inside the vagina. Pressing down on the abdomen at the same time, the doctor can check the uterus, ovaries and other organs.
Transvaginal ultrasound

Transvaginal ultrasound
During a transvaginal ultrasound, a healthcare professional or technician uses a wandlike device called a transducer. The transducer is inserted into your vagina while you lie on your back on an exam table. The transducer emits sound waves that generate images of your pelvic organs.
Hysteroscopy
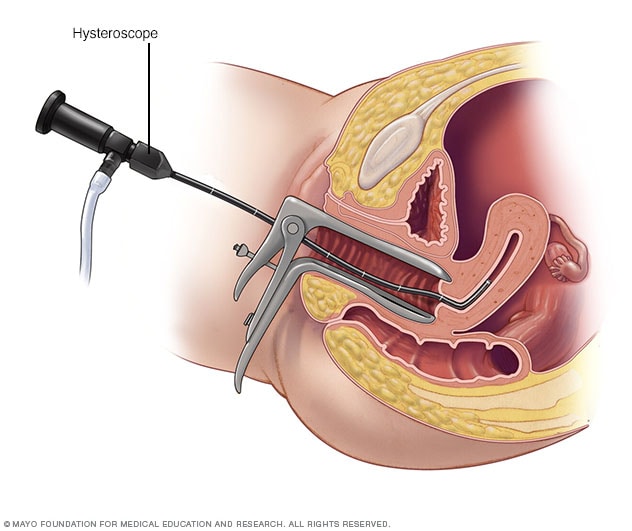
Hysteroscopy
During hysteroscopy (his-tur-OS-kuh-pee), a thin, lighted instrument provides a view of the inside of the uterus. This instrument also is called a hysteroscope.
Tests and procedures used to diagnose endometrial cancer include:
-
Examining the pelvis. A pelvic exam checks the reproductive organs. It's often done during a regular checkup, but it might be needed if you have symptoms of endometrial cancer.
During the exam, a health care professional carefully inspects the outer genitals. Two fingers of one hand are inserted into the vagina and the other hand presses on the abdomen to feel the uterus and ovaries. A device called a speculum is inserted into the vagina. The device opens the vaginal canal so the health professional can look for signs of cancer or other problems.
- Imaging tests. Imaging tests make pictures of the inside of the body. They can tell your health care team about your cancer's location and size. One imaging test might be a transvaginal ultrasound. In this procedure, a wandlike device called a transducer is inserted into the vagina. The transducer uses sound waves to create a video image of the uterus. The image shows the thickness and texture of the endometrium. Ultrasound can help your health care team look for signs of cancer and rule out other causes for your symptoms. Other imaging tests such as MRI and CT scans also may be suggested.
- Using a scope to examine your endometrium, called a hysteroscopy. During a hysteroscopy, a health care professional inserts a thin, flexible, lighted tube through the vagina and cervix into the uterus. This tube is called a hysteroscope. A lens on the hysteroscope allows the health professional to examine the inside of the uterus and the endometrium.
- Removing a sample of tissue for testing, called a biopsy. In an endometrial biopsy, a sample of tissue is removed from the lining of the uterus. Endometrial biopsy often is done in a health care professional's office. The sample is sent to a lab for testing to see if it is cancer. Other special tests give more details about the cancer cells. Your health care team uses this information to make a treatment plan.
- Performing surgery to remove tissue for testing. If enough tissue can't be obtained during a biopsy or if the biopsy results are unclear, you'll likely need to undergo a procedure called dilation and curettage, also called D&C. During D&C, tissue is scraped from the lining of the uterus and examined under a microscope for cancer cells.
If endometrial cancer is found, you'll likely be referred to a doctor who specializes in treating cancers involving the reproductive system, called a gynecologic oncologist.
Staging endometrial cancer
Once your cancer has been diagnosed, your health care team works to determine the extent of your cancer, called the stage. Tests used to determine your cancer's stage may include a chest X-ray, a CT scan, blood tests and positron emission tomography, also called a PET scan. Your cancer's stage may not be known until after you have surgery to treat your cancer.
Your health care team uses information from these tests and procedures to assign your cancer a stage. The stages of endometrial cancer are indicated using numbers ranging from 1 to 4. The lowest stage means that the cancer hasn't grown beyond the uterus. By stage 4, the cancer has grown to involve nearby organs, such as the bladder, or has spread to distant areas of the body.
More Information
Treatment
Endometrial cancer is usually first treated with surgery to remove the cancer. This may include removing the uterus, fallopian tubes and ovaries. Other treatment options may include radiation therapy or treatments using medicines to kill the cancer cells. Options for treating your endometrial cancer will depend on the characteristics of your cancer, such as the stage, your general health and your preferences.
Surgery
Treatment for endometrial cancer usually involves an operation to remove the uterus, called a hysterectomy. Treatment also usually includes the removal of the fallopian tubes and ovaries, called a salpingo-oophorectomy. A hysterectomy makes it impossible for you to become pregnant in the future. Also, once your ovaries are removed, you'll experience menopause if you haven't already.
During surgery, your surgeon also will inspect the areas around your uterus to look for signs that cancer has spread. Your surgeon also may remove lymph nodes for testing. This helps determine your cancer's stage.
Radiation therapy
Radiation therapy uses powerful energy to kill cancer cells. The energy can come from X-rays, protons or other sources. In certain situations, radiation therapy may be recommended before surgery. Radiation therapy can shrink a tumor and make it easier to remove.
If you aren't healthy enough to undergo surgery, you may opt for radiation therapy only.
Radiation therapy can involve:
- Radiation from a machine outside your body. During external beam radiation, you lie on a table while a machine directs radiation to specific points on your body.
- Radiation placed inside your body. Internal radiation, called brachytherapy, involves a radiation-filled device, such as small seeds, wires or a cylinder. This device is placed inside your vagina for a short period of time.
Chemotherapy
Chemotherapy uses strong medicines to kill cancer cells. Some people receive one chemotherapy medicine. Others receive two or more medicines together. Most chemotherapy medicines are given through a vein, but some are taken in pill form. These medicines enter the bloodstream and then travel through the body, killing cancer cells.
Chemotherapy is sometimes used after surgery to lower the risk that the cancer might return. Chemotherapy also can be used before surgery to shrink the cancer. This makes it more likely that the cancer is removed completely during surgery.
Chemotherapy may be recommended for treating advanced endometrial cancer that has spread beyond the uterus or to treat cancer that has come back.
Hormone therapy
Hormone therapy involves taking medicines to lower the hormone levels in the body. In response, cancer cells that rely on hormones to help them grow might die. Hormone therapy may be an option if you have advanced endometrial cancer that has spread beyond the uterus.
Targeted therapy
Targeted therapy uses medicines that attack specific chemicals in cancer cells. By blocking these chemicals, targeted treatments can cause cancer cells to die. Targeted therapy is usually combined with chemotherapy for treating advanced endometrial cancer.
Immunotherapy
Immunotherapy uses medicine that helps the body's immune system kill cancer cells. The immune system fights off diseases by attacking germs and other cells that shouldn't be in the body. Cancer cells survive by hiding from the immune system. Immunotherapy helps the immune system cells find and kill the cancer cells. For endometrial cancer, immunotherapy might be considered if the cancer is advanced and other treatments haven't helped.
Palliative care
Palliative care is a special type of health care that helps you feel better when you have a serious illness. If you have cancer, palliative care can help relieve pain and other symptoms. Palliative care is done by a team of health care professionals. This can include doctors, nurses and other specially trained professionals. Their goal is to improve the quality of life for you and your family.
Palliative care specialists work with you, your family and your care team to help you feel better. They provide an extra layer of support while you have cancer treatment. You can have palliative care at the same time as strong cancer treatments, such as surgery, chemotherapy or radiation therapy.
When palliative care is used along with all of the other appropriate treatments, people with cancer may feel better and live longer.
More Information
More Information
Clinical trials
Explore Mayo Clinic studies testing new treatments, interventions and tests as a means to prevent, detect, treat or manage this condition.
Coping and support
After you receive a diagnosis of endometrial cancer, you may have many questions, fears and concerns. Every person eventually finds a way to cope with an endometrial cancer diagnosis. In time, you'll find what works for you. Until then, you might try to:
- Find out enough about endometrial cancer to make decisions about your care. Find out enough about your cancer so that you feel comfortable about making treatment choices. Ask your health care team about the stage and your treatment options and their side effects. Ask your care team to recommend places you can go to get more information about cancer. Good sources of information include the National Cancer Institute and the American Cancer Society.
- Maintain a strong support system. Strong relationships may help you cope with treatment. Talk with close friends and family members about how you're feeling. Connect with other cancer survivors through support groups in your community or online. Ask your health care team about support groups in your area.
- Stay involved in your usual activities when you can. When you're feeling up to it, try to stay involved in your usual activities.
Preparing for your appointment
Make an appointment with a member of your care team or a gynecologist if you have symptoms that worry you. If you're diagnosed with endometrial cancer, you're likely to be referred to a doctor who specializes in cancers of the reproductive system, called a gynecologic oncologist.
Because appointments can be brief and there's often a lot to discuss, it's a good idea to be prepared. Here's some information to help you get ready, and what you can expect from your health care team.
What you can do
- Write down any symptoms you're experiencing, including any that might not seem related to the reason for your appointment.
- Make a list of all medicines, vitamins and supplements that you're taking. Also note if you've used any type of hormonal therapy in the past, including birth control pills, tamoxifen or other hormonal treatments.
- Ask a family member or friend to accompany you. Sometimes it can be difficult to remember all the information provided during an appointment. Someone who accompanies you may remember something that you missed or forgot.
- Write down questions to ask your health care team.
Your time with your health care professional is limited, so preparing a list of questions ahead of time can help you make the most of your time together. List your questions from most important to least important in case time runs out. For endometrial cancer, some basic questions to ask include:
- What's the most likely cause of my symptoms?
- Are there any other possible causes for my symptoms?
- What tests do I need to diagnose endometrial cancer?
- Are there other tests for staging the cancer?
- What treatments are available? What side effects can I expect from each treatment? How will these treatments affect my sexuality?
- What do you think is the best course of action for me?
- What are the alternatives to the primary approach that you're suggesting?
- I have other health conditions. How can I best manage them together?
- Are there any restrictions that I need to follow?
- Has my cancer spread? What stage is it?
- What's my prognosis?
- Should I see a specialist? What will that cost, and will my insurance cover it?
- Are there any brochures or other printed material that I can take with me? What websites do you recommend?
In addition to the questions that you've prepared, don't hesitate to ask additional questions during your appointment.
What to expect from your doctor
Be prepared to answer some questions about your symptoms. Questions may include:
- Have you experienced any unusual vaginal bleeding or discharge? How often does that occur?
- Do you have any pelvic pain?
- Have you had any other symptoms?
- Have your symptoms been continuous or occasional?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
- Have you taken estrogen-only hormone therapy for menopausal symptoms?
- Do you have any personal history of cancer?
- Have other members of your family been diagnosed with cancer? How old were your relatives when they were diagnosed? What types of cancer?