Diagnosis
Spirometer
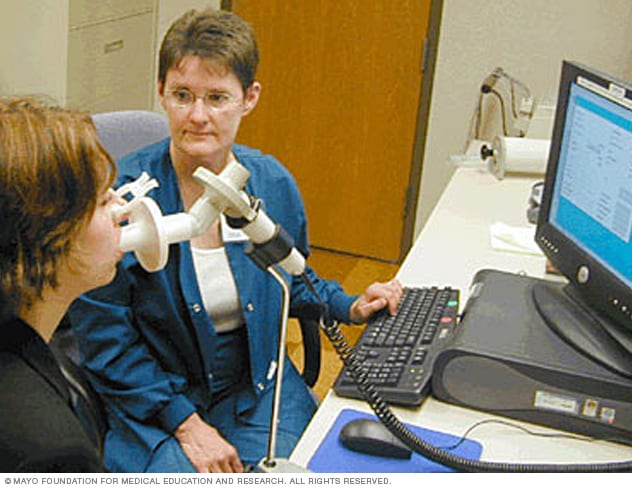
Spirometer
A spirometer is a diagnostic device that measures the amount of air you can breathe in and out and the time it takes you to breathe out completely after you take a deep breath.
During the first few days of illness, it can be difficult to distinguish the signs and symptoms of acute bronchitis from those of a common cold. During the physical exam, your doctor will use a stethoscope to listen closely to your lungs as you breathe.
In some cases, your doctor may suggest the following tests:
- Chest X-ray. A chest X-ray can help determine if you have pneumonia or another condition that may explain your cough. This is especially important if you smoke or have ever smoked.
- Sputum tests. Sputum is the mucus that you cough up from your lungs. It can be tested to see if you have illnesses that could be helped by antibiotics. Sputum can also be tested for signs of allergies.
- Pulmonary function test. During a pulmonary function test, you blow into a device called a spirometer, which measures how much air your lungs can hold and how quickly you can get air out of your lungs. This test checks for signs of asthma, chronic bronchitis or emphysema.
Treatment
Most cases of acute bronchitis get better without treatment, usually within a couple of weeks.
Medications
In some circumstances, your doctor may recommend other medications, including:
- Cough medicine. If your cough keeps you from sleeping, you might try cough suppressants at bedtime.
- Other medications. If you have allergies, asthma or chronic obstructive pulmonary disease (COPD), your doctor may recommend an inhaler and other medications to reduce inflammation and open narrowed passages in your lungs.
- Antibiotics. Because most cases of acute bronchitis are caused by viral infections, antibiotics aren't effective. However, if your doctor suspects that you have a bacterial infection, he or she may prescribe an antibiotic.
Therapies
If you have chronic bronchitis, you may benefit from:
- Pulmonary rehabilitation. This is a breathing exercise program in which a respiratory therapist teaches you how to breathe more easily and increase your ability to be physically active.
- Oxygen therapy. This delivers extra oxygen to help you breathe.
Lifestyle and home remedies
If you have bronchitis, to help you feel better, you may want to try the following self-care measures:
- Get enough rest. Rest and sleep help your body heal.
- Drink plenty of fluids. Staying hydrated can help to thin mucus.
- Avoid lung irritants. Don't smoke. Wear a mask when the air is polluted or if you're exposed to irritants, such as paint or household cleaners with strong fumes.
- Use a humidifier. Warm, moist air helps relieve coughs and loosens mucus in your airways. Be sure to clean the humidifier according to the manufacturer's recommendations to avoid the growth of bacteria and fungi in the water container.
- Consider a face covering in cold air. If cold air makes your cough worse and causes shortness of breath, put on a face mask or cover your mouth and nose with a scarf before you go outside.
Preparing for your appointment
You're likely to start by seeing your family doctor. If you have chronic bronchitis, you may be referred to a doctor who specializes in lung diseases (pulmonologist).
What you can do
Before your appointment, make a list of answers to the following questions:
- Have you recently had a cold or the flu?
- Have you ever had pneumonia?
- Do you have any other medical conditions?
- What medications, vitamins and supplements do you take regularly?
- Are you exposed to lung irritants at your job?
- Do you smoke or are you around tobacco smoke?
If possible, bring a family member or friend to your appointment. Sometimes it can be difficult to remember all the information provided. Someone who accompanies you may remember something that you missed or forgot.
If you've ever seen another physician for your cough, tell your present doctor what tests were done. If possible, bring the reports with you, including results of a chest X-ray, sputum culture and pulmonary function test.
What to expect from your doctor
Your healthcare professional is likely to ask you several questions, such as:
- When did your symptoms begin?
- Have your symptoms been continuous or occasional?
- Do your symptoms affect your sleep or work?
- Does anything improve or worsen your symptoms?
- Does cold air bother you?
- Do you notice that you wheeze sometimes?
- Have you had bronchitis before? Has it ever lasted more than three weeks?
- In between bouts of bronchitis, have you noticed that you're more short of breath than you were a year earlier?
- Do you exercise? Can you climb one flight of stairs without difficulty? Can you walk as fast as you used to?
- Do you smoke? If so, how much and for how long?
- Have you inhaled recreational drugs?
- Have you received the annual flu shot?
- Have you ever been vaccinated against pneumonia? If so, when?