Overview
Merkel cell carcinoma
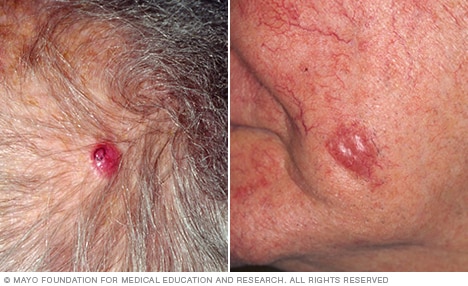
Merkel cell carcinoma
Merkel cell carcinoma is a rare type of skin cancer. It most often appears as a bump on the face, heard or neck.
Merkel cell carcinoma is a rare type of skin cancer. It most often appears as a bump on the face, head or neck. Merkel cell carcinoma also is called neuroendocrine carcinoma of the skin.
Merkel cell carcinoma most often happens in people older than 50. Long-term sun exposure or a weakened immune system may raise the risk of getting this cancer.
Merkel cell carcinoma tends to grow fast and to spread quickly to other parts of the body. Treatment may depend on whether the cancer has spread beyond the skin.
Products & Services
Symptoms
The first symptom of Merkel cell carcinoma most often is a growth on the skin. This skin cancer can happen anywhere on the body. It happens most often on skin that typically gets sunlight. In white people, the growth is most likely to be on the head or neck. In Black people, the growth more often is on the legs.
A Merkel cell carcinoma can cause:
- A bump on the skin that often is painless.
- A bump that grows quickly.
- A bump whose two sides don't match.
- A bump that looks pink, purple, red-brown, or the same color as the skin around it.
When to see a doctor
Make an appointment with a healthcare professional if you have a mole, freckle or bump that changes size, shape or color. Also see a healthcare professional if you have a bump that grows fast or bleeds easily after minor injury, such as washing your skin or shaving.
Causes
It's often not clear what causes Merkel cell carcinoma.
This skin cancer happens when cells in the skin develop changes in their DNA. A cell's DNA holds the instructions that tell the cell what to do. In healthy cells, the DNA gives instructions to grow and multiply at a set rate. The instructions tell the cells to die at a set time.
In cancer cells, the DNA changes give other instructions. The changes tell the cancer cells to grow and multiply at a fast rate. Cancer cells can keep living when healthy cells would die. This causes too many cells.
The cancer cells might form a mass called a tumor. The tumor can grow to invade and destroy healthy body tissue. In time, cancer cells can break away and spread to other parts of the body. When cancer spreads, it's called metastatic cancer.
Merkel cell carcinoma is named for the cells where experts once thought it started. The Merkel cells are found at the bottom of the outer layer of skin. The Merkel cells are connected to the nerve endings in the skin that play a role in the sense of touch. Healthcare professionals no longer believe that this cancer starts in the Merkel cells. They don't know exactly what kind of cells it starts in.
It's often not clear what causes the DNA changes that lead to Merkel cell carcinoma. Researchers have found that a common virus plays a role in causing Merkel cell carcinoma. The virus, called Merkel cell polyomavirus, lives on the skin. It doesn't cause symptoms. Experts don't know exactly how this virus causes Merkel cell carcinoma.
Risk factors
Factors that may raise the risk of Merkel cell carcinoma include:
-
Skin that sunburns easily. Anyone of any skin color can get Merkel cell carcinoma. But it's more common in people who have less melanin in their skin. Melanin is a substance that gives color to skin. It also helps protect the skin from damaging rays from the sun.
People with Black or brown skin have more melanin than do people with white skin. So white people are more likely to get Merkel cell carcinoma than are people with Black or brown skin.
- Too much UV light. Ultraviolet light, also called UV light, raises the risk of Merkel cell carcinoma. UV light can come from the sun. Being in the sun without covering the skin with clothing or sunblock raises the risk of Merkel cell carcinoma. UV light for treatment of the skin condition psoriasis also can raise the risk of this skin cancer.
- Tanning bed use. People who use indoor tanning beds have a higher risk of Merkel cell carcinoma.
- A weakened immune system. People with weakened immune systems are more likely to get Merkel cell carcinoma. A weakened immune system can happen in people with certain health conditions, such as HIV infection and chronic leukemia. It also can happen in people taking certain medicines, such as medicines that lower the immune response.
- History of other skin cancers. Merkel cell carcinoma is linked to other skin cancers, such as basal cell carcinoma and squamous cell carcinoma.
- Older age. The risk of Merkel cell carcinoma goes up with age. This cancer is most common in people older than age 50, though it can happen at any age.
Complications
Even with treatment, Merkel cell carcinoma often spreads to other parts of the body. When cancer spreads, healthcare professionals sometimes say it metastasizes. Merkel cell carcinoma tends to travel first to nearby lymph nodes.
Later it may spread to the brain, bones, liver or lungs. It can keep these organs from working as they should. Cancer that spreads is harder to treat and can be fatal.
Prevention
While exposure to sunlight isn't proved to cause all Merkel cell carcinomas, it is thought to be a risk factor for this cancer. Getting less sun exposure may lower your risk of skin cancer.
Try to:
Stay out of the sun in the middle of the day
For much of North America, the sun's rays are strongest between about 10 a.m. and 3 p.m. Plan to be outdoors at other times of the day, even during winter or when the sky is cloudy. When outside, stay in the shade as much as possible.
Wear sunscreen year-round
Use a broad-spectrum sunscreen with an SPF of at least 30, even on cloudy days. Apply sunscreen generously. Reapply every two hours, or more often if you're swimming or sweating.
Wear protective clothing
To protect your skin from the sun, wear dark, tightly woven clothes that cover the arms and legs. Wear a wide-brimmed hat that shades the face and ears.
Don't forget sunglasses. Look for sunglasses that block both types of ultraviolet light, also called UV light, that comes from the sun. The two types are UVA and UVB.
Check your skin often
Look at your skin often for new growths or changes in moles, freckles, bumps and birthmarks. Use mirrors to check your face, neck, ears and scalp. Report any changes to your healthcare professional.
Even though Merkel cell carcinoma most often is on the face, head and neck, look at other areas of your body. Look at your chest and trunk and the tops and undersides of your arms and hands. Look at the front and back of your legs and your feet. Look at the bottom of the feet and the spaces between your toes. Also check your genital area and between your buttocks.
Jan. 10, 2025