Diagnosis
Diagnosing hyperhidrosis may start with your health care provider asking about your medical history and symptoms. You may also need a physical exam or tests to further evaluate the cause of your symptoms.
Lab tests
Your health care provider may recommend blood, urine or other lab tests to see if your sweating is caused by another medical condition, such as an overactive thyroid (hyperthyroidism) or low blood sugar (hypoglycemia).
Sweat tests
Sweat test
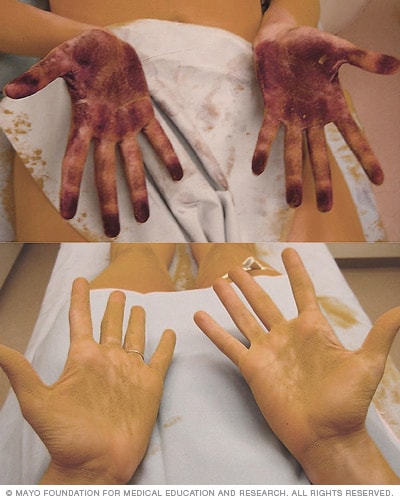
Sweat test
Moisture-sensitive powder indicates the presence of heavy sweating (top) compared with hands after surgery to treat hyperhidrosis (bottom).
Or you may need a test that pinpoints the areas of sweating and evaluates how severe your condition is. Two such tests are an iodine-starch test and a sweat test.
Treatment
Treating hyperhidrosis may start with treating the condition causing it. If a cause isn't found, treatment focuses on controlling heavy sweating. If new self-care habits don't improve your symptoms, your health care provider may suggest one or more of the following treatments. Even if your sweating improves after treatment, it may recur.
Medications
Drugs used to treat hyperhidrosis include:
-
Prescription antiperspirant. Your health care provider may prescribe an antiperspirant with aluminum chloride (Drysol, Xerac AC). Apply it to dry skin before going to bed. Then wash the product off when you get up, taking care to not get any in your eyes. Once you start seeing results from using it daily for a few days, you can scale back to once or twice a week to maintain the effect.
This product can cause skin and eye irritation. Talk with your health care provider about ways to reduce side effects.
- Prescription creams and wipes. Prescription creams that contain glycopyrrolate may help hyperhidrosis that affects the face and head. Wipes soaked in glycopyrronium tosylate (Qbrexza) may ease symptoms of the hands, feet and underarms. Possible side effects of these products include mild skin irritation and dry mouth.
- Nerve-blocking medications. Some pills (oral medications) block the nerves that trigger sweat glands. This can reduce sweating in some people. Possible side effects include dry mouth, blurred vision and bladder problems.
- Antidepressants. Some medications used for depression can also decrease sweating. They may also help decrease anxiety.
-
Botulinum toxin injections. Treatment with botulinum toxin (Botox) blocks the nerves that trigger the sweat glands. Most people don't feel much pain during the procedure. But you may want your skin numbed beforehand. Your health care provider might offer one or more of the methods used to numb skin. These include topical anesthesia, ice and massage (vibration anesthesia).
Each affected area of your body will need several injections. It may take a few days to notice results. To retain the effect, you'll likely need repeat treatments about every six months. A possible side effect is short-term muscle weakness in the treated area.
Surgical and other procedures
Your health care provider might suggest other treatments:
-
Iontophoresis. With this home treatment, you soak your hands or feet in a pan of water while a device passes mild electric current through the water. The current blocks the nerves that trigger sweating. You can buy the device if you have a prescription from your health care provider.
You'll need to soak the affected areas for 20 to 40 minutes. Repeat the treatment 2 to 3 times a week until your symptoms improve. After you get results, you can reduce treatments to once a week or once a month to maintain the effect. Talk with your health care provider if you experience side effects.
- Microwave therapy. With this therapy, a handheld device (miraDry) delivers microwave energy to destroy sweat glands in the armpits. Treatments involve two 20- to 30-minute sessions, three months apart. Possible side effects are a change in skin sensation and some discomfort. Long-term side effects are unknown.
- Sweat gland removal. If you sweat heavily only in your armpits, your health care provider may suggest removing those sweat glands. This may be done through scraping them away (curettage), suctioning them out (liposuction) or using a combination of the two (suction curettage).
-
Nerve surgery (sympathectomy). During this procedure, the surgeon removes a small section of the spinal nerves that control sweating in your hands. A possible side effect is permanent heavy sweating in other areas of your body (compensatory sweating). Surgery is generally not an option for isolated head and neck sweating. A variation on this procedure treats the palms. It interrupts the nerve signals without removing the sympathetic nerve (sympathotomy), which reduces the risk of compensatory sweating.
Because nerve surgery has a risk of side effects and complications, it is usually only considered for people who have tried many other treatments without good results.
Each of these procedures may be done with general anesthesia or with local anesthesia and sedation.
Lifestyle and home remedies
The following suggestions may help control sweating and body odor:
- Use antiperspirant. Antiperspirants containing 6% to 20% aluminum chloride (Drysol, Xerac AC, others) can temporarily block sweat pores. This reduces the amount of sweat that reaches the skin. This type of product may help with minor hyperhidrosis. Apply it to dry skin before going to bed and wash it off when you wake.
- Choose shoes and socks made of natural materials. Shoes made of natural materials, such as leather, allow your feet to breath, which helps prevent sweaty feet. Wear moisture-wicking athletic socks when you're active. In the store, you can tell which socks are moisture wicking by reading the packaging.
- Keep your feet dry. Change socks or hose one or two times a day. Dry your feet each time. If you wear pantyhose, try the type with cotton soles. Use shoe insoles and foot powder to help absorb sweat. Wear sandals or go barefoot when you can. Or at least slip out of your shoes now and then.
- Choose clothing to suit your activity. When you can, wear natural fabrics, such as cotton, wool and silk. These allow your skin to breathe. When you're very active, you might prefer fabrics designed to wick moisture away from your skin.
Coping and support
Hyperhidrosis can be the cause of discomfort and embarrassment. You may have trouble working or enjoying recreational activities because of wet hands or feet or wet stains on clothing. You might feel anxious about your symptoms and become withdrawn or self-conscious. You may be frustrated or upset by other people's reactions.
Talk about your concerns with your health care provider, a counselor or a medical social worker. Or you may find it helpful to talk with other people who have hyperhidrosis.
Preparing for your appointment
You may start by seeing your primary care provider. You may then be referred to a specialist in diagnosing and treating conditions of the hair and skin (dermatologist). If your condition is not responding to treatment, you may be referred to a specialist in the nervous system (neurologist) or a surgeon.
Here's some information to help you get ready for your appointment.
What you can do
Before your appointment, you might want to list answers to the following questions:
- Has anyone in your immediate family ever had similar symptoms?
- Does your sweating stop when you're asleep?
- What medications and supplements do you take regularly?
- Have your symptoms caused you to avoid social situations or activities?
What to expect from your doctor
Your health care provider is likely to ask you several questions, such as:
- When did the heavy sweating begin?
- Where on your body does it occur?
- Have your symptoms been continuous or occasional?
- What, if anything, seems to improve your symptoms?
- What, if anything, appears to worsen your symptoms?
Oct. 25, 2024